The decision to get a dental implant is an important one — both from a medical and financial perspective. Understanding what the procedure involves, how to prepare, what to expect, and how recovery works will help you make an informed decision and achieve the best results.
This guide covers everything: from the initial evaluation and contraindications, to what happens on the day of surgery and what life with a dental implant looks like.
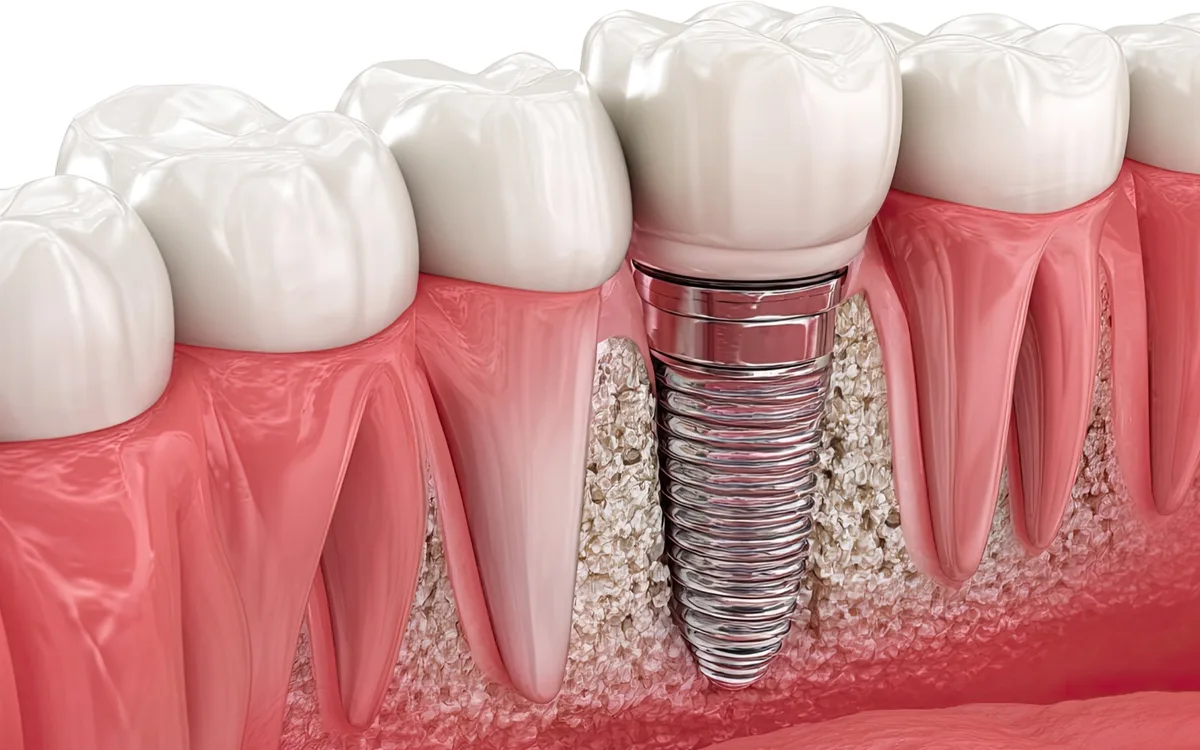
Medical Evaluation Before an Implant
Before any implant procedure, the clinician will perform a comprehensive evaluation that includes:
Clinical Examination
- Assessment of the overall condition of the oral cavity
- Analysis of remaining teeth, gingiva, and occlusion (how the teeth meet)
- Oral hygiene evaluation — poor hygiene must be corrected before implant placement
- Identification of infection foci (teeth with granulomas, active periodontitis)
Imaging Studies
- Panoramic X-ray (OPG) — provides an overview of both jaws, sinuses, and important anatomical structures
- CBCT (Cone Beam CT) — 3D tomography with reduced radiation doses, essential for precise measurement of available bone in height, width, and density
- CBCT is not optional — it is the minimum diagnostic standard for proper implant planning
Blood Tests
The clinician may request:
- Complete blood count
- Blood glucose and HbA1c (for diabetic patients)
- Coagulation panel (for patients on anticoagulant therapy)
- Calcium and vitamin D levels (in selected cases)
General Health Assessment
Inform your clinician about:
- All medications you are taking
- Chronic diseases (diabetes, hypertension, heart disease, osteoporosis)
- Allergies (to medications, to metals — although titanium allergy is extremely rare)
- Smoking — how many cigarettes per day, for how many years
- Previous dental treatments and experiences with anesthesia
When You Cannot Get a Dental Implant
There are absolute and relative contraindications. It is important to know them:
Absolute Contraindications
These make implant placement impossible or extremely risky:
- Recent radiation therapy in the head and neck area — high risk of osteoradionecrosis. A waiting period of at least 12–24 months after completing radiation therapy is recommended, with individualized assessment.
- Active treatment with intravenous bisphosphonates (zoledronic acid, pamidronate) — risk of medication-related osteonecrosis of the jaw (MRONJ). Oral bisphosphonates (for osteoporosis) carry a lower risk but require careful evaluation.
- Severe hematological diseases with major uncontrolled coagulation disorders
- Severe immunosuppression — transplant recipients on strong immunosuppression, active chemotherapy
Relative Contraindications (Manageable)
These require additional caution but do not automatically rule out implant placement:
- Diabetes mellitus — if well controlled (HbA1c < 7–8%), implant success rates are comparable to non-diabetic patients. Uncontrolled diabetes significantly increases the risk of failure.
- Smoking — smokers have a 5–10% higher failure rate. Reducing or quitting smoking 2–4 weeks before and after the procedure significantly improves prognosis.
- Bruxism (teeth grinding) — does not contraindicate the implant but requires wearing a night guard after prosthetic placement.
- Active periodontal disease — must be treated and stabilized before implant placement. Untreated periodontitis is a major risk factor for peri-implantitis.
- Insufficient bone — not a contraindication but a solvable problem through bone augmentation or sinus lift.
Types of Dental Implants
Endosseous Implants (Standard)
These account for over 95% of implants used today. They are inserted directly into the jawbone, have a screw shape, and are made from:
- Titanium (most common) — biocompatible, excellent osseointegration, used for over 50 years
- Zirconia (ceramic) — an option for patients who want a 100% metal-free solution, aesthetically superior in the front area where the gingiva is thin
Subperiosteal Implants
Placed on the bone surface, under the periosteum (the membrane covering the bone). They are used extremely rarely, only in cases of severe bone atrophy where augmentation is not possible. They do not represent the current standard of treatment.
Zygomatic Implants
Inserted into the zygomatic bone (cheekbone), used in cases of severe maxillary atrophy where there is insufficient bone for conventional implants and augmentation is not feasible. They are an advanced alternative for All-on-4 type rehabilitations.
Complete Timeline: From Consultation to Final Tooth
Week 0: Consultation and Diagnosis
- Clinical examination, CBCT, treatment plan
- Discussion about options, prices, timeline
- Signing the informed consent
Weeks 1–2: Preparation (If Needed)
- Treatment of cavities or infection foci
- Professional scaling and cleaning
- Possible extraction of the compromised tooth (with a 6–8 week healing period, or immediate placement)
Day of Surgery: Implant Insertion
- The procedure is performed under local anesthesia (identical to what is used for fillings)
- Conscious sedation is available for anxious patients
- Duration: 30–60 minutes per implant
- Gingival incision, preparation of the bone site with progressively sized drills, implant insertion, suture
Months 1–6: Osseointegration
This is the critical phase during which the implant “fuses” with the bone. Osseointegration means the formation of direct contact between the titanium surface of the implant and newly formed bone — without any intermediate tissue.
- Mandible (lower jaw): osseointegration in 2–3 months (bone is denser)
- Maxilla (upper jaw): osseointegration in 4–6 months (bone is less dense)
After Osseointegration: Prosthetic Phase
- Uncovering the implant (a small incision to expose the healing abutment)
- Impression (digital or conventional)
- Fabrication of the definitive crown in the lab (7–14 days)
- Crown fixation on the implant (cementation or screw retention)
What to Expect on the Day of Surgery
Before the Procedure
- Eat a light meal 2 hours before
- Take prescribed medications (usually a prophylactic antibiotic 1 hour before)
- Avoid alcohol for 24 hours prior
- Wear comfortable clothing
During the Procedure
- You will be fully awake but will not feel pain thanks to anesthesia
- You will feel pressure and vibrations — this is normal
- Communication with the clinician is possible throughout
- Duration: 30–60 minutes per implant (simple cases)
Immediately After the Procedure
- Anesthesia lasts 2–4 hours
- You will receive written postoperative care instructions
- Do not drive if you received conscious sedation
- Apply ice externally, 15 minutes every hour, for the first 6 hours
Postoperative Care
First 24 Hours
- Ice — cold compresses on the cheek, 15 minutes with 15-minute breaks, to reduce swelling
- Do not rinse and do not spit forcefully — the blood clot may be dislodged
- Liquid or semi-liquid diet — warm soup (not hot), yogurt, purees
- Do not smoke — smoking compromises healing
- Medication: antibiotic (if prescribed), anti-inflammatory (ibuprofen 400–600 mg every 8 hours), paracetamol if needed
First Week
- Soft food — pasta, rice, boiled eggs, ground meat, bananas, avocado
- Oral hygiene — gentle brushing in the rest of the mouth, avoiding the implant area. Gentle rinsing with chlorhexidine 0.12% twice daily
- Swelling peaks at 48–72 hours, then gradually subsides
- Bruising may appear on the cheek — this is normal and disappears within 7–10 days
- Suture removal — at 7–14 days
First Month
- Gradual return to normal diet
- Avoid very hard or crunchy foods in the implant area
- Continue careful oral hygiene
- Follow-up with the clinician at 2 weeks
Pain — What Is Normal and What Is Not
Normal
- Mild to moderate discomfort in the first 3–5 days, manageable with ibuprofen or paracetamol
- Tenderness to pressure in the implant area for 1–2 weeks
- Moderate swelling, peaking on days 2–3
Warning Signs — Contact Your Clinician
- Intense pain that worsens after day 3–4 (instead of improving)
- Fever above 38.5 degrees C persisting for more than 24 hours
- Pus discharge from the surgical site
- Active bleeding that does not stop with gentle compression after 30 minutes
- Persistent numbness of the lip or chin (possible nerve injury)
- The implant feels mobile
How Long Until You Can Eat Normally?
- Day 0–3: Liquids and semi-liquids (soup, smoothie, yogurt)
- Days 3–7: Soft foods (pasta, rice, eggs, fish)
- Weeks 2–4: Semi-solid foods (soft meat, cooked vegetables)
- After 1 month: Almost everything, avoiding only very hard foods directly on the implant area
- After definitive prosthetic placement: Normal diet, without significant restrictions
Osseointegration — The Essential Process
Osseointegration is the biological process by which bone forms in direct contact with the implant surface, creating a solid and stable bond. It was first described by Prof. Per-Ingvar Branemark in the 1960s and remains the foundation of all modern implantology.
What Influences Osseointegration?
- Primary stability — how tightly the implant sits in the bone immediately after insertion
- Bone quality — dense bone (anterior mandible) integrates faster than cancellous bone (posterior maxilla)
- Implant surface — modern surfaces (SLA, TiUnite, Xpeed) accelerate osseointegration
- Smoking — reduces blood flow at the bone level, slowing healing
- Uncontrolled diabetes — affects bone metabolism
- Overloading — premature forces on the implant can prevent osseointegration
What Can You Do to Promote Osseointegration?
- Do not smoke (or reduce to a minimum) for at least 4 weeks before and after the procedure
- Keep blood glucose under control if you are diabetic
- Follow the soft diet for the recommended period
- Do not press on the implant area with your tongue or removable denture
- Take prescribed supplements (vitamin D, calcium, if indicated)
Follow-up Schedule
An implant does not end at insertion. Monitoring is essential:
| Time point | What is checked |
|---|---|
| 2 weeks | Soft tissue healing, suture removal |
| 1 month | Clinical evaluation, possible X-rays |
| 3 months | Osseointegration assessment (mandible) |
| 4–6 months | Osseointegration assessment (maxilla), start of prosthetic phase |
| 6 months after prosthetic placement | First routine check-up |
| Annually | Clinical check-up + periapical X-ray |
Conclusion
A dental implant is a routine procedure in modern dentistry, with success rates exceeding 95%. Adequate preparation, choosing an experienced clinician, following postoperative instructions, and adhering to the follow-up schedule are the factors that make the difference between a good result and an excellent one.
If you are considering a dental implant, the first step is a consultation with an implantology specialist who will evaluate your clinical situation and propose a personalized treatment plan. Find a specialist in the ClickDent clinic directory or request a personalized evaluation directly.
